Information on Masks in the Coronavirus Pandemic—All in One Place

Please note that this article is for informational purposes only. Individuals should consult their health care provider before following any of the information provided.
More and more individuals are receiving the vaccine for COVID-19, the disease caused by the coronavirus. Does this mean they can stop wearing masks?
No, according to the Centers for Disease Control and Prevention’s (CDC) frequently asked questions about vaccination. Wearing a mask remains important, even after vaccination. To make that decision, public health researchers and experts need to understand more about the protection provided by the COVID-19 vaccine.
Keep reading for information from the CDC, Johns Hopkins Medicine, the U.S. Food and Drug Administration (FDA) and others below.
Are Masks Effective Against the Coronavirus Disease?
Wearing a mask can be an effective way to prevent transmission, especially when combined with other preventative measures, like hand-washing and physical distancing. Masks act as a barrier between an individual’s mouth and nose and their environment and can lessen the amount of respiratory droplets released into the air.
Based on the knowledge that these droplets play a role in spreading the coronavirus and scientific evidence that masks reduce the spray of droplets, the CDC recommends wearing a mask in public settings and in places where maintaining six feet of distance from others (who do not live in your household) is not possible.
Read more about masks here: CDC Calls on Americans to Wear Masks to Prevent COVID-19 Spread, CDC and Coronavirus Face Masks & Protection FAQs, Johns Hopkins Medicine.
Safest Masks to Buy and Wear
Different types of masks have different levels of aerosol filtration efficiency, or the percentage of airborne particles of a certain size that would be blocked by the mask’s material. An N95 respirator, for example, is named for its ability to filter out at least 95% of airborne particles, according to a CDC infographic on blue surgical masks versus N95 respirators (PDF, 226.97 KB).
Non-Medical Mask Filtration Efficiency
Researchers tested the effectiveness of various fabrics commonly used in cloth masks in an April 2020 study published in ACS Nano, a peer-reviewed, scientific journal from the American Chemical Society. To conduct the experiment, researchers pushed aerosolized particles through each material being tested.
For a respiratory infection like COVID-19, droplets below 5 μm are thought to be the “primary source of transmission,” according to the authors. Therefore, researchers examined particles sized between approximately 10 nm and 6 μm. Unless otherwise indicated, the following values assume the mask is properly fitted. Percentages refer to the particles blocked by a particular fabric.
Type of Cloth
Fabrics with tighter weaves, higher threads per inch (TPI) and lower porosity performed better—meaning they blocked a higher percentage of particles sized within the study’s target range (10 nm to 6 μm) from passing through.

Cotton fabric with 600 threads per inch (TPI) prevented transmission of about 98.4% of particles, while 80 TPI-cotton only prevented 14%.
Layering Materials
Layering cloth fabrics can help to create a more effective mask, even for materials with a low thread count.
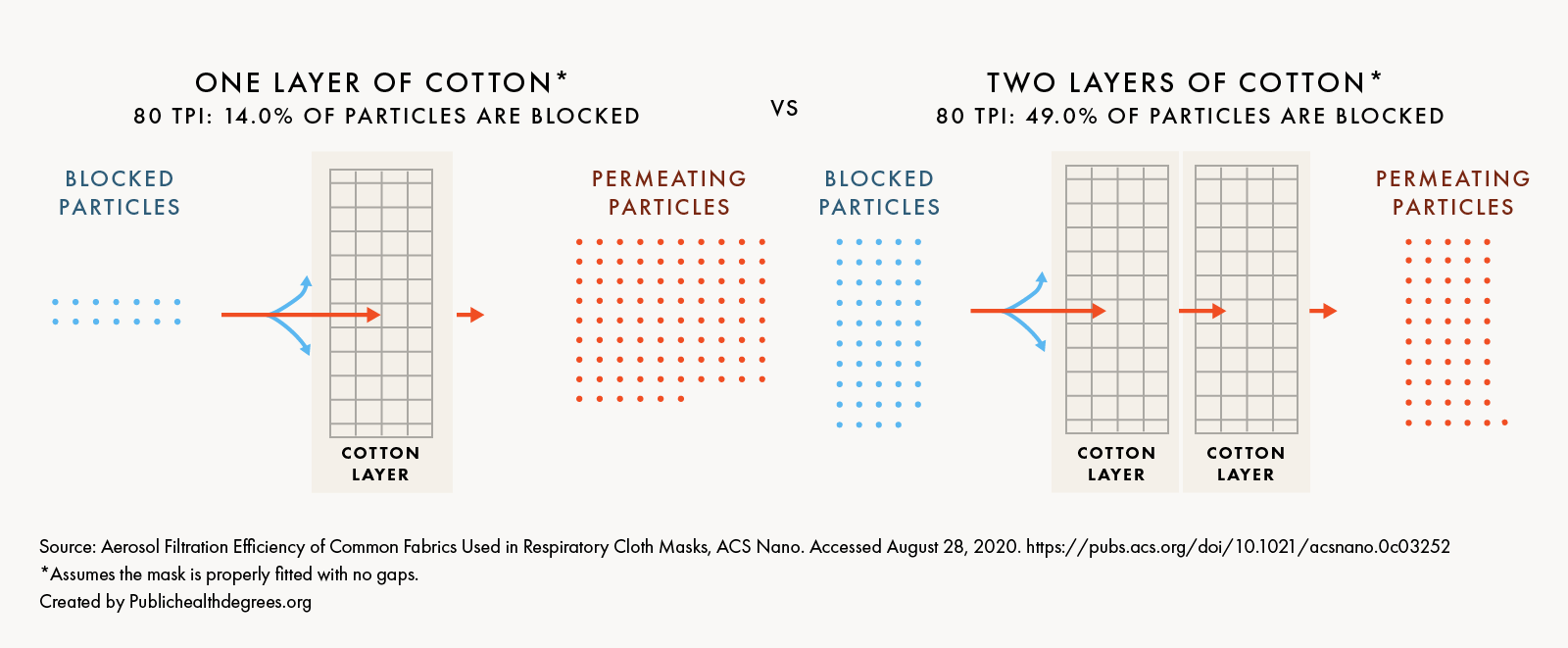
Two layers of 80 TPI-cotton blocked 49% of particles compared to 14% for only one layer of the same fabric.
Mixing Fabrics
Research suggests that combining materials to create a hybrid mask, such as high thread-count cotton and silk, can make a better filter.

A hybrid cotton/silk mask performed better than two layers of 80 TPI-cotton, 98.5% to 49%.
Fitting the Mask Well
Improperly fitted masks create gaps between the mask and face that allow air to “leak” out, reducing the mask’s effectiveness. Masks should fit snugly while still allowing exhaled air to be vented.
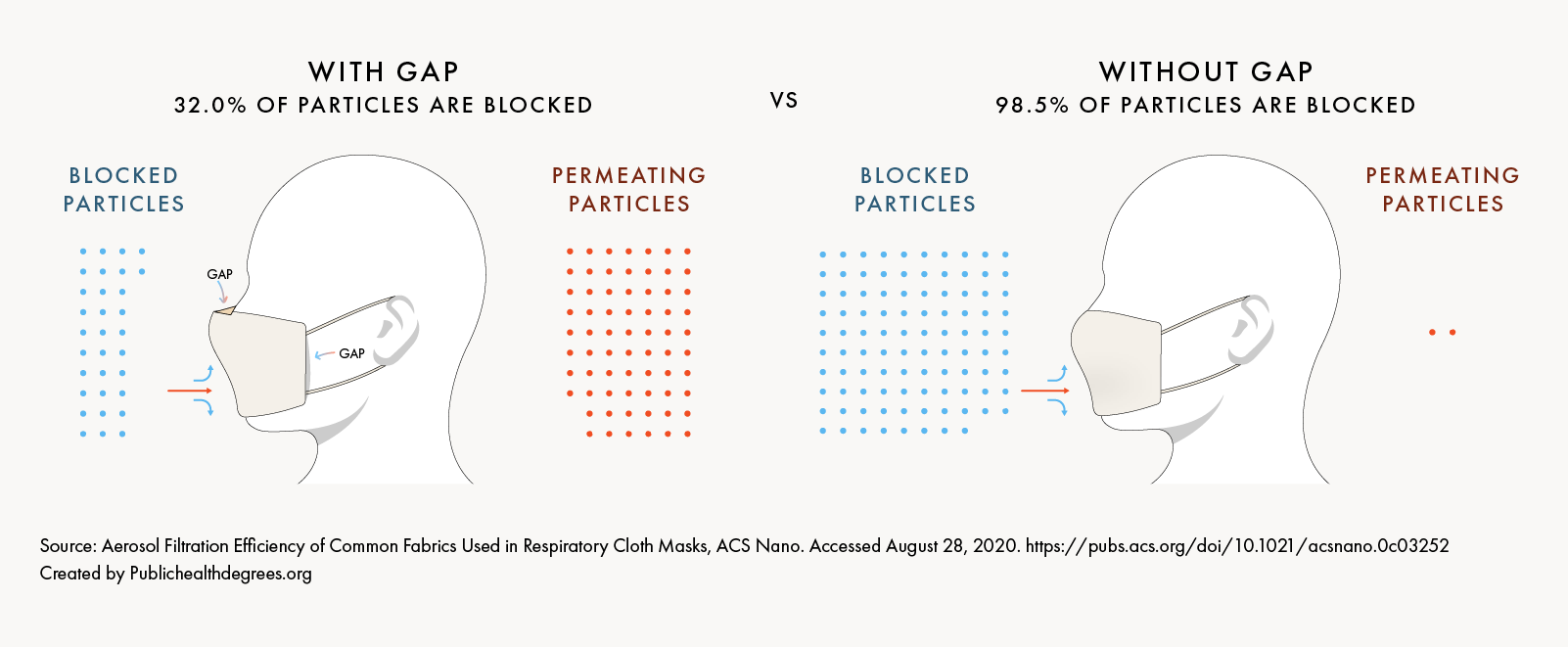
When a hybrid cotton/silk mask was fitted with a gap, it only blocked 32% of particles, compared to 98.5% particles blocked in the same mask with no gap.
Inspired by the CDC’s How to Select, Wear, and Clean Your Mask, other questions to ask when choosing a mask include:
- Will this mask cover my face properly? (A mask should fully cover the nose and mouth.)
- Is the material thick enough to be effective? (Consult the April 2020 study published in ACS Nano to learn more about specific materials).
- Is this mask intended for health care personnel? (N95 and surgical masks should be reserved for providers on the front lines.)
- Does this mask have an exhalation valve or vent? (These let particles escape and are not CDC-recommended.)
- Is there scientific evidence to support this mask’s effectiveness? (Note that the effectiveness of gaiters and face shields is not known; as of August 2020, they are still being evaluated.)
Who Should Wear a Mask?

Masks should be worn by:
- Individuals age 2 and older in public settings.
- Those who suspect they have COVID-19.
- Those who know they have COVID-19.
- Caregivers of people with COVID-19.

Masks should not be worn by:
- Children younger than age 2.
- Individuals who have trouble breathing.
- Individuals who cannot remove a mask without help.
When to Wear a Mask
The CDC highlights three key times for putting on a mask—in addition to when required by state or local authorities:
In public settings
When sick and interacting with others at home
Interacting with someone sick at home
Source: Key Times to Wear a Mask, CDC
To better understand when to wear a mask in specific situations, including work, playing sports, hotels, travel and more, visit the CDC’s COVID-19: Daily Activities and Going Out page.
Masks and Exercising
Because they make it difficult to breathe easily, masks should not be worn while exercising outdoors, according to the World Health Organization. Try to keep a distance of one meter (the CDC’s typical recommendation is six feet) between yourself and others while exercising.
How to Wear Masks
A cloth mask should cover the nose and mouth and be secured under the chin. It should fit snugly against the sides of the face but still allow the wearer to breathe easily.
To learn more about wearing masks and creating your own, visit:
- ASL Video Series: Use of Cloth Face Coverings to Help Slow the Spread of COVID-19, CDC: tutorial video in American Sign Language (ASL) on how masks help and how to make one at home
- COVID-19: Uso de Cubiertas de Tela Para la Cara, CDC: tutorial video in Spanish for making a mask using everyday items
- How to Properly Wear a Face Mask, Johns Hopkins Medicine: infographic of best practices for mask wearing
- How to Wear Masks, CDC: visualizations and best practices for wearing and removing a mask
How to Wash Masks

Cloth masks and other fabric face coverings should be cleaned after each use and can typically be washed on the warmest possible temperature setting with regular laundry detergent. Allow to air-dry or toss in the clothes dryer at the highest heat setting. They can also be washed by hand with a disinfecting bleach solution. The CDC’s mask-cleaning guidance recommends soaking the mask in one of the following solutions for five minutes and rinsing with water:
- 5 tablespoons household bleach per gallon of room-temperature water
- 4 teaspoons household bleach per quart of room-temperature water
Disposable blue surgical masks cannot be cleaned and should be tossed when visibly soiled or damaged, according to Johns Hopkins Medicine’s advice on mask care.

N95 respirator masks are typically worn only once. However, the FDA issued Emergency Use Authorizations (EUAs) for “the emergency use of decontamination systems” to decontaminate certain respirators used by health care personnel when supplies are insufficient during the coronavirus pandemic. Research on decontaminating medical-grade N95 masks has also suggested that a 50-minute treatment in an electric cooker without pressure at 212 degrees Fahrenheit can be effective. However, this is experimental research, and further studies of reusing respirators are needed.
How to Make Masks More Comfortable
Face coverings can feel uncomfortable at times, especially in warmer weather. Below, find tips for feeling better wearing a mask.
Avoiding Foggy Glasses
- Wash lenses with soapy water and allow to air-dry before putting on a mask.
- Try antifogging solutions used for ski goggles and scuba masks.
- Place a folded tissue between your mouth and the mask.
- Make sure the top of your mask is tight and the bottom a little looser.
To read more, visit AARP’s “Face Masks Can Prove Tricky for Those With Eyeglasses.”
Dealing With the Heat
- Be strategic about going outside, especially if you have a respiratory condition. Can you combine trips? Can someone else go for you? Can the trip be delayed until later in the day?
- Watch for signs of heat illness or exhaustion in yourself and others. Symptoms include dizziness, lightheadedness, dehydration and a racing heartbeat. If these happen, get out of the heat, safely remove the mask and get medical care.
- Check that your home’s cooling system is fully functional.
- Choose a breathable material. Cotton masks are both breathable and effective; blue surgical masks may also feel better.
- Keep an extra clean and dry mask on hand to swap out if yours becomes sweaty or uncomfortable.
To read more, visit How to Stay Cool While Wearing a Mask, Penn Medicine and COVID-19 Story Tip: The Important of Staying Cool While Wearing a Mask Outside in the Summer Heat, Johns Hopkins Medicine.
More Tips for Better Comfort
- To get used to breathing with a mask, start slow. Wear the mask at home for a short time. Later, wear it on a short walk, and gradually increase your time.
- If ear loops cause discomfort, try a mask that ties in the back (also called an “ear saver”).
- Look into a face mask bracket, which is a plastic frame that goes under the mask and creates space between your mouth and the material.
To read more, visit COVID-19: How Much Protection Do Face Masks Offer?, Mayo Clinic.
Face Mask Policies and the Americans With Disabilities Act (ADA)
The coronavirus pandemic ushered in a wave of mandates and ordinances from state and local governments requiring individuals to wear masks in particular settings, often in public indoor spaces and within six feet of others outside the home.
While helpful for preventing spread, these regulations have also created questions. Wearing a mask may not be feasible for everyone, including people who have disabilities that make wearing or removing a mask impossible. Businesses may refuse services to people without masks, but those with disabilities are protected from discrimination by the Americans with Disabilities Act (ADA).
How do mask mandates and the ADA interact? Consider the official guidance below.
Contrary to inaccurate posts on the web and social media, the Department of Justice clarified that the ADA “does not provide a blanket exemption to people with disabilities from complying with legitimate safety requirements necessary for safe operations,” according to a press release on June 30, 2020.
The ADA and Face Mask Policies, Disability Issues Brief
Businesses and government agencies may require patrons to wear a mask, based on CDC guidance. However, statewide mask mandates “do not override the consideration of reasonable modifications required by the Americans with Disabilities Act,” according to an August 20, 2020, post in Disability Issues Brief.
Reasonable modifications should be considered to allow the person with a disability to participate in the programs offered or goods and services provided. Questions that businesses and agencies can ask include:
- Can customers wear a scarf, loose face covering or full-face shield?
- Can customers order online or by phone for curbside pickup or no-contact delivery in a timely manner?
- Can the client wait in the car for an appointment and enter the building when contacted?
- Can appointments be offered by phone or video call?
Mask Exemptions During the COVID-19 Pandemic—A New Frontier for Clinicians, JAMA Health Forum
A masking exemption is one form of reasonable modification but not the only one. “Amid a global pandemic, reasonable accommodations for masking intolerance can and should include avoidance measures, such as curbside services and delivery,” wrote this article’s authors.
In the workplace, employers can legally require mask-wearing, and workers may be asked to provide medical documentation to receive an exemption. However, the report continues, workplace accommodations “should be conceptualized in a broader framework than a simple mask exemption.” Accommodations could also include working remotely, moving to a non-public-facing position or leaving under certain conditions.
Please note that this article is for informational purposes only. Individuals should consult their health care provider before following any of the information provided.
Information last updated January 2021
